Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
In the healthcare industry, providers’ top priority is bringing the best quality care to their patients. But this comes not only with treating patients; it also requires effective administrative strategies and clinical functions so that practitioners are properly reimbursed for their services. It helps to keep the doors open and the light on so healthcare providers can help everyone.
Here the revenue management cycle comes under the spotlight. There are a multitude of factors that help the healthcare industry, but RCM ensures practitioners are properly and quickly reimbursed. However, this is not only beneficial to providers but equally beneficial to patients.
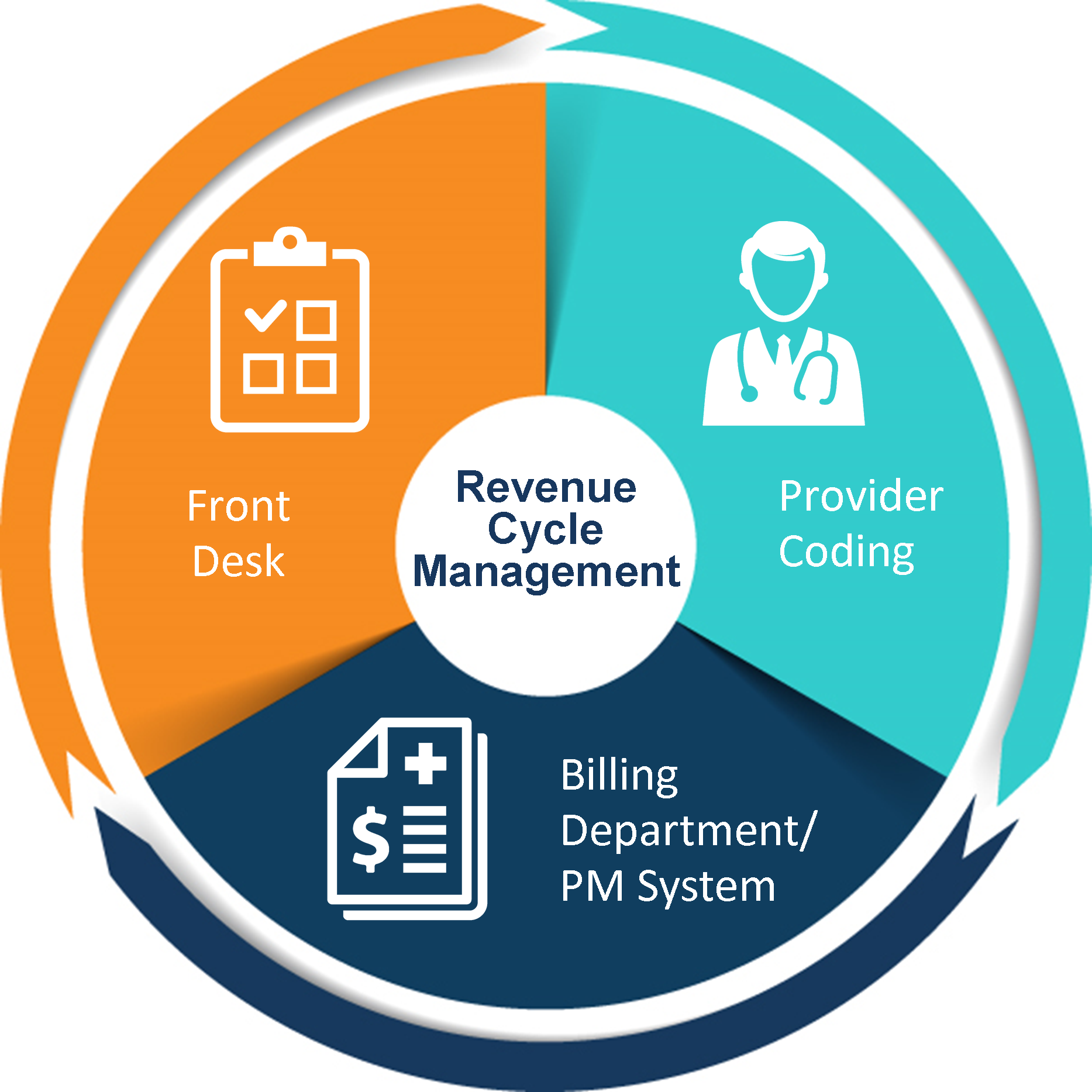
Before jumping into the pool of RCM benefits, let’s discuss the primary steps involved in Revenue Cycle Management:
Revenue Cycle Management
Revenue cycle management is the process where healthcare facilities, practitioners, and small practices can ensure they’ll get reimbursed for their services as quickly as possible. It is a complex process, managing many parts and players. It is the process of handling claims, processing payments, and generating revenue in the healthcare industry. It begins when a patient makes an appointment and ends with receiving the patient’s payment or writing off the bills.

Steps in the Healthcare Revenue Cycle
Prior authorization and Eligibility Verification
The healthcare provider collects information about the patient to establish his account. It includes patient insurance information and verifies insurance eligibility. RCM focuses attention on completing the patient intake steps accurately. Ineligible insurance or inaccurate information can be the result of denied claims in the revenue cycle. It means a delay occurs in the provider’s reimbursement payments.
Charge Capturing and Coding
Charge capturing is the process by which medical services are documented and translated into billable charges using standardized medical codes. The procedure codes play a pivotal role in helping insurance companies determine reimbursement amounts.
Without accurate medical coding, insurers might delay the patient’s claim, so this result may delay provider reimbursement. It not only costs the provider time and money but also reinvestigates the denied time and appeals again.
Claims Submission
When a patient’s medical services have been properly coded, the claim is sent to the insurance company for further approval. RCM makes sure the claim submission process happens quickly by tracking and managing the claim from the start of the process properly.
Payment Collection
After the patient’s claim approval, the insurer reimburses the practitioner based on the patient’s eligibility. If there is any remaining balance left after the insurance reimbursement, it becomes the healthcare provider’s responsibility to reach out to the patient and collect payment from the patient.
Medical Service Review
Effective RCM stimulates healthcare providers to analyze clinical treatment data. This analysis empowers providers to pinpoint the stage in revenue cycle management where errors occur and discover ways to reduce costs. Consequently, this will enhance practitioners’ revenue and elevate the quality of patient experience.
Benefits of Revenue Cycle Management
Let’s have a look at the most noteworthy benefits of revenue cycle management:
#1 Raise in Claims Paid after First Submission
Effective revenue cycle management increases focus on properly completing front-end tasks to make sure claims are paid the first time they’re submitted. Included tasks are insurance verification, the collection of correct patient information, and proper coding.
On average, the denied claims ratio is five to ten percent after the first submission. However most of the denials are because of human errors and technical problems. Mostly, errors occur in coding and insurance verification, or information is missing from the patient’s chart. The fact is that 90% of claim denials are preventable.
Denial claims moved like a tennis ball between insurance companies and healthcare providers for months untill issues were resolved. The only way to avoid delays is to make sure claims are properly checked before they are submitted.
#2 Raise in Practice Collection and Revenue
Healthcare facilities face a large number of financial responsibilities. They not only cover the cost of patient care services but also pay their staff for the work they do. When claims are denied and patients cannot make upfront payments. It causes delays in healthcare providers’ income, posing challenges in managing their finances.
To handle these challenges, Revenue Cycle Management (RCM) plays a pivotal role in discovering recurring patterns of claim denials. By understanding these patterns, practitioners can take proactive measures to prevent claim denials in the near future, ensuring they receive reimbursement in a timely manner.
Because of claim denials, providers not only face delayed reimbursement but also suffer higher expenses for investigations and appeals. Approximately every year $15,000 spent on reworking claims.
#3 Increased Emphasis on Quality Care
When healthcare practitioners implement revenue cycle management, they no longer need to spend time and money correcting errors and appealing claims. Practices can switch these resources toward increasing the quality of care.
Furthermore, RCM facilitates the transition of healthcare providers from traditional fee-for-service reimbursement models to value-based reimbursement practices.
Value-Based Reimbursement
In value-based reimbursement, practice goals are providing better care for patients by enhancing the practice of service over the quantity of service.
#4 Improved Patient Experience
Effective RCM improves the overall patient experience by giving more importance to patient care. Patients demand fines and comprehensive healthcare, reducing their likelihood of re-admittance.
Revenue Cycle Management makes clear processes like scheduling, filling out intake forms, and billing to develop a satisfactory experience for both patients and administrative staff. It also gives importance to insurance verification upfront, so patients will better understand their insurance eligibility from the start.
#5 Reduce Administrative Burden
This is the administrative staff’s responsibility to schedule the appointment, establish or update patient information, and verify their insurance. By implementing revenue cycle management, front-end tasks are streamlined so the administrative staff can work efficiently.


